What is Sciatica? Do I have it?
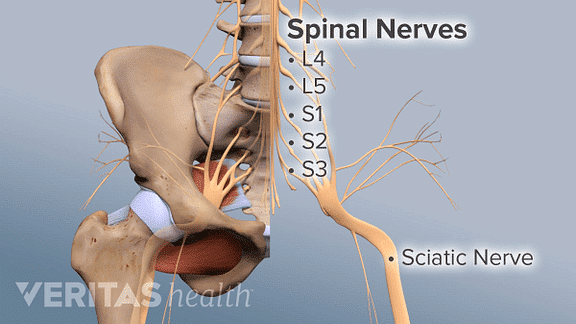
The sciatic nerve is the largest and thickest nerve in the body. It is formed from the union of 5 nerve roots (L4-S3) and travels down the back of the leg into the foot. Its purpose is to innervate the muscles, skin and other connective tissue down the leg. When one or more of these nerve roots is irritated, the associated pain in the leg and the back along the path of the nerve, is diagnosed as Sciatica. It is one of the most common types of pain as up to 40% of people experience it during their lifetime. The pain can be described as sharp, shooting, tingling, and sometimes as a deep ache. It is usually only down one leg but it can occur bilaterally. The pain can present in the glute, hamstring, calf, or foot. Sciatica doesn’t always present with back pain.
Sciatica could occur for a number of different reasons. It could occur from prolonged and repetitive movements which compress or stretch the nerves. Acute compression or tensile forces could also irritate the nerve. This includes a bulging or herniated disc or narrowing of the intervertebral space. Sciatica can often be mistaken for other issues in the back including SI joint pain, herniated discs, lumbar radiculopathy, and spinal stenosis. It is possible to have these issues with sciatica and so it is good to be assessed by a physical therapist to be differentially diagnosed, and to distinguish between these problems. A common finding with sciatica is positive nerve tension. There are tests which put the sciatic nerve on stretch or provide tension to the nerve which will reproduce the pain. These tests include the straight leg test, cross straight leg test, and the slump test.
If you are diagnosed with sciatica is it important to know that even with the pain you are experiencing, research shows that you will get better with a non-pharmacological approach. Usually imaging including an X-ray or an MRI is not needed. Sciatica can be managed with the help of physical therapists. Conservative treatment includes avoiding aggravating motions, education, exercise, and time to heal. When symptoms last greater than 6 weeks without improvement with physical therapy, or are getting worse including experiencing neurological deficits such as numbness and weakness, then a further assessment will be required by a physician.
As part of conservative treatment, sciatica often responds well to improving strength and motor control of the hips and trunk (core). Low back pain may also show positional preference. Some people may feel better sitting leaning forward, in a flexed position. Other people may feel better leaning back, standing, or walking. If after being in these positions the pain starts to move away from the limb and moves closer to the spine, this is called centralization. This is a good sign and means the neural desensitization is occurring. If pain moves further from the spine with one of these motions, it is called peripheralization and you would not want to continue that particular motion.
A physical therapist can assess your issue and come up with a differential diagnosis. If it is sciatica, we can prepare a plan that is tailored best for you. Having a better understanding of the issue will allow you to manage and care for the problem with the goal of alleviating pain.
In good health,
Jeffrey Walsh PT, DPT, CFMT
References and Image credit:
https://www.health.harvard.edu/pain/sciatica-of-all-the-nerve#:~:text=Sciatica%20is%20one%20of%20the,more%20frequent%20as%20you%20age
https://www.health.harvard.edu/pain/sciatica-a-to-z
https://www.spine-health.com/conditions/sciatica/sciatic-nerve-and-sciatica
https://www.spine-health.com/conditions/sciatica/what-you-need-know-about-sciatica
#teamcynergy #physicaltherapy #sciatica #sciaticapain #sciaticarelief #backpain #sports #sportsperformance #getmovingkeepmoving #sportsinjuryrehab #strengthandconditioning #injuryprevention #clinicalathlete #functionalmovement #nike #getpt1st #sportsrehab #physiotherapy #physicaltherapynyc #equinox #acl #aclrecovery #chooseptfirst #we💜healingourpatients #cynergyphysicaltherapy #ny #cynergypt #performance #physicaltherapists #movement #movementismedicine
